Identifying and Diagnosing EoE
Identifying patients who should be further evaluated for eosinophilic esophagitis (EoE) can be challenging. Some individuals have a higher risk of EoE based on family history and ancestry, male sex, and comorbid atopic disease.1,2
Evidence is accumulating that environmental factors, premature or cesarean birth, early antibiotic exposure, food allergy, lack of breast feeding, and lack of early microbial exposure are also linked to development of EoE.2
Clinical manifestations of EoE, which are largely attributed to esophageal dysfunction from epithelial remodeling, can be non-specific and may vary depending on several factors, including endotype, duration of disease, and patient age.4 Symptoms in pediatric patients include nausea, vomiting and abdominal pain, while adolescents and adults are more likely to present with dysphagia, heartburn, food impaction, and regurgitation (Table 1).5
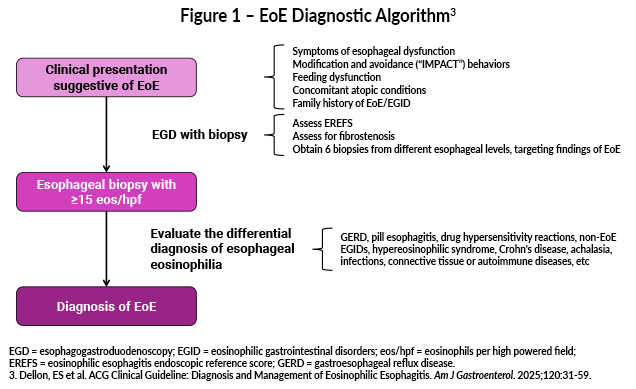
EoE reference score, EREFS representing Edema, Rings, Exudate, Furrows and Stricture is used for endoscopic findings. Patients suspected of having EoE undergo esophagogastroduodenoscopy (EGD) to assess the extent of eosinophilic infiltration. Diagnostic criteria and other conditions with associated esophageal eosinophilia are listed in Table 1. Patients who have ≥15 eosinophils/high-powered field should be evaluated for EoE.6 EoE is patchy – at least 6 biopsies are needed at 2 esophageal levels in any patient with dysphagia.3 Of note, failure of a trial of proton pump inhibitors (PPI) is no longer part of the diagnostic criteria for EoE. Differentiating between EoE and GERD can be particularly challenging due to the similarity in their clinical signs.
References
- Khan S, Guo X, Liu R, et al. An update on eosinophilic esophagitis: Etiological factors, coexisting diseases, and complications. Digestion. 2021;102:342-356. doi:10.1159/000508191
- Lyles J, Rothenberg M. Role of genetics, environment, and their interactions in the pathogenesis of eosinophilic esophagitis. Curr Opin Immunol. 2019;60:46-53. doi:10.1016/j.coi.2019.04.004
- Dellon, ES et al. ACG Clinical Guideline: Diagnosis and Management of Eosinophilic Esophagitis. Am J Gastroenterol. 2025;120:31-59.
- Chen JW. Management of eosinophilic esophagitis: Dietary and nondietary approaches. Nutr Clin Pract. 2020;35(5):835-847. doi:10.1002/ncp.10571
- Muir A, Falk GW. Eosinophilic esophagitis: A review. JAMA. 2021;326(13):1310-1318. doi:10.1001/jama.2021.14920
- Dellon ES, Liacouras CA, Molina-Infante J, et al. Updated international consensus diagnostic criteria for eosinophilic esophagitis: Proceedings of the AGREE conference. Gastroenterol. 2018;155(4):1022-1033.e10. doi:10.1053/j.gastro.2018.07.009